[ad_1]
Discussion
Referring providers have been criticised for writing poor-quality referrals for many years.1–3 This study identified inconsistencies and ambiguities within Canadian referral guidelines. No referral data type was consistently identified for inclusion by all referral guidelines. Surprisingly, only 7 of 13 (54%) referral guidelines specifically recommended the patient’s name and 8 of 13 (62%) recommended the patient’s contact information, be included in the referral. The remaining guidelines either made no recommendation21 or generally specified ‘patient information’.22 23 We propose that the lack of consensus and specificity in referral guidelines contributes to why referring providers unintentionally omit essential referral data, leading to low-quality referrals.
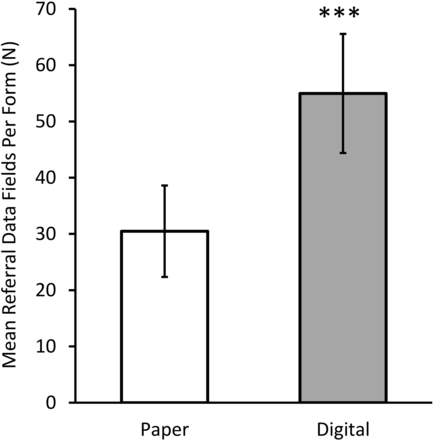
To our knowledge, this study presents the first characterisation of referral data fields from clinically used referral forms across multiple specialties. The requested referral data should contain all clinically relevant information that consultants need.24 We, therefore, used this data to codesign a standardised referral form with referring providers, consultants and administrators as recommended by the Canadian Medical Association.8 Codesign participants wanted referral forms to be short and simple; however, this study demonstrated that newer digital referral forms requested more information from referring providers. One potential reason why digital referral forms are longer and more complex is because digital referrals are not restricted to a single physical sheet of paper. Limiting digital referral form length is important because additional referral data does not correlate with consultants’ confidence in triaging appointments.25 Referral form length will also increase administrative burdens for referring and consultant providers, which correlates with provider burnout13 14 and intention to stop practicing.15 Therefore, we recommend that consultants’ providers adopt shorter, standardised, evidence-based referral forms, such as the one codesigned here.
The codesign of this referral form is a step toward providing clearer referral guidelines to improve referral quality. Some studies have recommended that referring providers require more training on how to write referrals,4 26 however, a Cochrane review from 2008 identified that education alone is insufficient.27 Instead, we recommend following England’s National Health Services’ Sustainability Model, creating interventions that target processes, staff education and organisational improvements.28 The Cochrane review concluded that clear referral guidelines (staff education) released in conjunction with a referral form (process change) can significantly improve referral quality.27
A randomised trial in Norway also demonstrated that a combination of provider education and referral form improves referral quality.29 However, the Norwegian referral form was based on disease-specific clinical guidelines and consultant opinion. The codesign approach used in this study facilitated dialogue between referring providers, consultant providers and administrators, leading to more nuanced learning. Specifically, the codesign participants highlighted that specifying referral data fields is only one part of the problem. Participants expected high-quality referral forms to be brief, reduce administrative burdens, leverage technology to facilitate form completion and only request referral data that facilitate consultant triage. These finding came organically from the codesign open forum and there is increasing awareness of the value that codesign brings to digital health technology development.30 Given these findings, it is possible that previous efforts to standardise referral forms have failed because without codesign, referral forms tend towards being longer, more complex and request information that referring providers do not have or is better collected directly from patients.
The next step from this study is to further implement the codesigned referral form in clinical practice. Additionally, we recommend revision to existing referral guidelines to provide clearer direction for referring and consulting providers. Once this is completed, then further quality improvement cycles may be completed to further refine and define the components of high-quality referrals and referral forms.
Strengths and limitations
The main limitation of this study was that all reviewed referral forms and codesign participants were from Ontario. We attempted to mitigate any local practice patterns by collecting forms from all geographic regions within Ontario. However, there may be difference in the referral data that consultants require in different regions. Codesign participants also expressed this concern and suggested that the codesigned referral form could be customised for different regions as needed to assist with referral triage or decision-making. Additionally, this study only assessed referral forms for consultation requests. Accordingly, these findings and the codesigned referral form will not be adequate for all referral types, such as diagnostic, home care, allied health or laboratory services. Finally, the referral form review was completed by a single author due to study constraints. However, each codesign participant had the opportunity to review and discuss these findings, which should mitigate potential biases in the primary outcome—the codesigned referral form.
[ad_2]
Source link