[ad_1]
Discussion
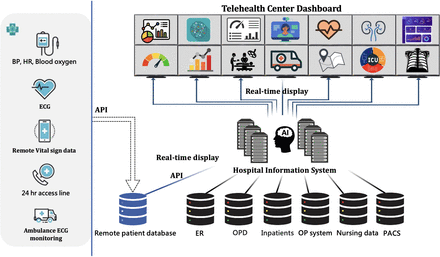
We demonstrated the successful implementation of the multidisciplinary telehealth platform at TCVGH, which serves as a hub for networking hospitals. Using this innovative system-integrated platform, we have improved consultation efficiency and lowered access barriers. Additionally, this web-based telehealth platform enhanced emergency response and the quality of care, as reflected by the reduced non-emergency referrals and improved patient adherence. The AI-powered monitoring platform enhances diagnostic accuracy and predicts significant arrhythmias in post-stroke patients. Providing timely alerts enables telecare nurses to take proactive measures, reducing the risk of stroke recurrence.
In addition to integrating multiple functions into a unified platform, our centre has also pioneered several innovative approaches in advanced telehealth domains. One of these initiatives involves providing long-term, real-time continuous ECG monitoring for at-risk patients in a home setting. Continuous ECG monitoring enables the early detection of rare but potentially fatal heart rate abnormalities, allowing timely physician intervention to prevent serious cardiac events. AFib is the most recognised factor for cryptogenic stroke. Traditionally, physicians used 14-day Holter ECG recordings to identify high-risk AFib cases; however, the data could only be reviewed when the patient returned to the clinic 2 weeks later, delaying potential diagnosis and intervention.2 To enhance real-time care, our centre pioneered continuous ECG monitoring to track the postdischarge status of stroke patients for up to 30 days, identifying an additional proportion of arrhythmia patients and offering timely medical support.
The experience of our integrated telehealth platform is on par with, if not superior to, the telemedicine practices in countries with long-standing expertise in this field. The Cleveland Clinic’s virtual care centre operates 24/7, offering integrated services across multiple specialties including remote intensive care unit monitoring and real-time ambulance telemetry.3 Their system has shown improved patient outcomes through coordinated virtual care delivery and rapid specialist access.4 Mayo Clinic’s connected care centre has pioneered advanced remote patient monitoring systems that integrate with home health devices and provide virtual emergency services.5 In Asia, Singapore General Hospital has implemented a sophisticated telehealth command centre that coordinates virtual specialist rounds, emergency vehicle telemedicine and chronic disease monitoring.6 These centres have demonstrated the benefit of integrating telehealth care. However, implementation approaches vary based on regional regulations and infrastructure capabilities.
Telehealth in the European Union (EU) further emphasises the collaboration of cross-border eHealth services. Specialty care integration has been supported by initiatives like the eHealth Digital Service Infrastructure, which comprises 17 partners from 10 European countries, facilitating cross-border health data exchange and projects like e-Mental Health Innovation and Transnational Implementation Platform, which deploys a combined digital and face-to-face mental health programme in North Western Europe. However, issues with interoperability, language barriers, reimbursement and quality control remain.7–9 Addressing the legal, regulatory and funding barriers to establishing a unified digital health infrastructure and enhancing care accessibility remains a critical next step.10
Limitation
This study has several limitations that should be carefully considered. First, the observational case study at a single centre lacks a control group and randomisation, making it difficult to attribute observed outcomes solely to the telehealth intervention. Potential confounding factors, including the global healthcare system improvements during the study period, might have influenced the results. First, selection bias may occur because the participating institutions and patients were selected based on geographic accessibility and technological readiness, limiting the generalisability of our findings to broader populations. Variability in technological infrastructure and inconsistent internet connectivity in rural and mountainous regions further confound the outcomes. Moreover, differences in digital literacy among HCPs and patients could influence user experiences, satisfaction levels and adoption rates, potentially biasing satisfaction survey results. This survey specifically focused on rural and underserved regions, which may introduce selection bias and limit the generalisability. The use of self-reported satisfaction questionnaires may introduce response biases, such as social desirability or recall bias, which could lead to overinflated satisfaction ratings. Lastly, due to the limited observation period, this study primarily assessed immediate and short-term outcomes rather than long-term health outcomes or detailed cost-effectiveness evaluations. Further studies with longer observation time, broader patient populations and standardised technology frameworks are essential to validate these initial findings and fully understand the telehealth platform’s long-term impact.
[ad_2]
Source link