[ad_1]
Discussion
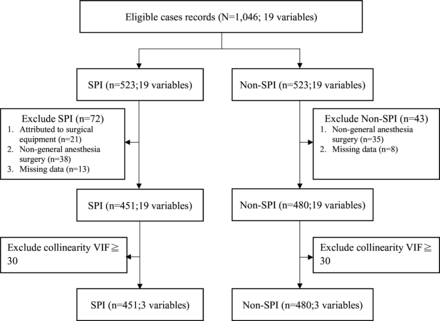
This study developed and validated a predictive model for SPIs using retrospective data from 931 surgical patients under general anaesthesia. The sample size was determined based on practical considerations, using all eligible cases available during the study period, as a priori power calculation was not feasible in this retrospective design. To assess the sample size sufficient for LR modelling, we adopted the criteria proposed.22 The final model yielded a shrinkage factor of 0.976 and an adjusted Nagelkerke’s R² of 0.177. With 451 SPI outcome events and three candidate predictors, the events per variable was 150.3. These indicators collectively support the adequacy of the sample size for developing a robust prediction model. Future prospective studies will incorporate formal sample size and power calculations to further strengthen the study design and generalisability.
Key predictors, including BMI, CCI and number of medication types, align with prior research linking patient characteristics, comorbidities and medication used to increase SPI risk. In addition, findings indicate a higher SPI risk in male patients, emphasising the need for gender-sensitive prevention strategies. Previous studies have noted sex-related disparities in health outcomes due to factors like disease susceptibility, healthcare access and socioeconomic influences.23 In addition to patient characteristics, intraoperative factors, such as surgical positioning, anaesthesia duration, fluid management, blood loss and temperature fluctuations, further contribute to SPI risk. The use of medical devices, such as headrests and armboards, along with patient transfer, friction, shear forces and postoperative immobility, further elevates SPI risk.3 4 8 24
This study confirmed that high BMI, elevated CCI, multiple medication types and male sex are independently associated with increased SPI risk. The operating room environment may also play a role, with the SPI group showing higher temperatures (23.26°C±0.74) and elevated humidity levels (56.41%±1.20) compared with the non-SPI group (22.16°C±0.63 and 55.04%±1.33). These findings suggest that suboptimal thermal management may increase tissue vulnerability. Evidence indicates that skin temperature rises by 1.6°C after 45 min of surgery,25 with further increases if surgery extends beyond 120 min.26 27 Elevated skin temperature can compromise skin structure and function, while low ambient temperatures reduce blood flow, heightening SPI risk. Increased humidity may weaken skin integrity, promoting friction.28 Although temperature and humidity were statistically significant in univariate analyses, they were excluded from the final model due to limitations in data quality. This exclusion reflects a consistent approach in our model development—prioritising the inclusion of predictors with reliable measurement and clinical applicability, rather than statistical significance alone.
The predictive model demonstrated varying performance levels across LR, MLP and DT models. Among the models tested, MLP achieved the highest performance, with an AUC of 0.836, accuracy of 0.773, precision of 0.812, recall of 0.688 and an F1 score of 0.745. Its ability to capture complex non-linear relationships underscores its potential for accurate SPI prediction. In contrast, the LR model, with an AUC of 0.707, showed lower recall and F1 scores, suggesting reduced effectiveness in identifying SPI cases. The DT model demonstrated moderate performance but struggled with high-dimensional, nonlinear data, making it less effective than MLP.
Given its superior performance, the MLP model could be integrated into clinical decision support systems for real-time SPI risk stratification within electronic health records. Its high sensitivity and accuracy support early SPI detection, facilitating timely intervention, optimising resource allocation and improving preventive strategies. Future research should aim to scale these predictive models across diverse surgical settings to improve patient safety and perioperative care quality.
[ad_2]
Source link