[ad_1]
Discussion
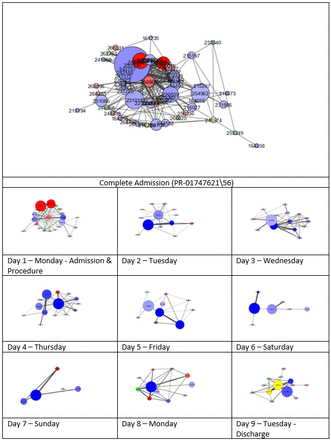
The findings of this study have demonstrated that the variation in the structure of HCP daily networks, as described by their network metrics, can be used to visualise the changes in a patient’s intensity of care during a hospital admission.
By breaking down admission-based HCP patient interaction networks into daily networks opens up the possibility of investigating a number of issues in more depth. Two key areas for further study would be issues related to weekday versus weekend working patterns: second, comparisons of the intensity of care and its relationship to the prediction of length of stay post procedure. Care must be taken when considering this level of analysis that patients are at similar stages of their care when compared.
Previous publications on the theme of HCP collaboration and patient interaction such as Zheng et al,3 Malin et al4 and Soulakis et al,5 are focused on organisational structures, applying analytical techniques developed for social media to apply to the collaboration structures of HCPs in a hospital.
Later publications began to focus on the level of care patients were being given, Yao et al,14 considered a random cohort of 100 patients and demonstrated that graph analysis could distinguish different care patterns for individual patients. This study also considered the different graph analytical metrics and how they could be used to indicate different aspects of care. Kim et al15 compared directly care patterns with length of stay.
Yan et al16 compared the level of care of patients with and without COVID-19 in the ICU. This study used events from their EPR system but differentiated between proactive events, for example, clinical notes, medication and laboratory orders and reactive, events such as medication administrations focusing on the former and ignoring the latter. Zhu et al,17 took a similar approach by splitting their HCPs into core teams, support teams and administrative teams. Kahn et al18 was focused on collaboration at the patient bedside, meaning that medication administrations and laboratory test collection were the type of event used.
Little temporal analysis has taken place within this theme with one exception Durojaiye et al6 considered the diurnal differences in multidisciplinary care teams.
It should be noted that this method is highly applicable to any healthcare site running an EPR system that incorporates a pipeline for data extraction for research. The base data structure for creating the daily networks could be as simple as patient ID, HCP ID, professional’s professional group and the datetime stamp of the action. This minimum data requirement should be available from any EPR system irrespective of its vendor or common data model (eg, Observational Medical Outcomes Partnership Common Data Model (OMOP CDM) or RDV).
This base data structure represents a bi-partite graph with patients and professionals representing the two node sets and the datetime stamp creating the edge. The monopartite network required for the analysis is simply a projection of the bi-partite network, using the 60 min period as the inferred relationship. This projection would be difficult to achieve with a traditional database approach as this is a self-referencing relationship.19
Similarly, the coding for this project was completed in Python and iGraph but similar results could be achieved using the networkX package20 or other programming environments (such as R), or the graph data science module in Neo4j.21 The network metrics used to distinguish the different network structure are the base metrics available in any network analysis environment.
The current study describes a novel and generalisable method that can be applied to routinely collected EPR data extracted for research using graph analytics, with a proof-of-concept demonstrator and associated metrics. It also provides a data-driven approach to explore wider clinical and operational applications within a healthcare setting. For example, determining expected HCP interactions by day following a procedure, in order to optimally plan staffing and resource allocation; identifying deviation(s) from normal HCP-–patient interactions for early identification of potential complications for risk of increased length of stay; HCP interaction patterns as markers of adverse events or for additional monitoring and understanding of infectious disease outbreaks within hospital areas.
By breaking down admission-based HCP patient interaction networks into daily networks opens up the possibility of investigating a number of issues related to weekday versus weekend working patterns. Care must be taken when considering this level of analysis that patients are at similar stages of their care when compared.
Further research is required to understand the optimal interpretation of analytical metrics in this context and to determine interaction patterns across a range of clinical scenarios. Nevertheless, the general approach described is applicable irrespective of a particular EPR system, and is potentially scalable independently of healthcare system, geography, patient group or population. It is anticipated that the use of graph analytics will become standard practice for investigation of multiple issues in relation to healthcare and provides an additional approach to address specific questions that are difficult or impossible to determine using other methods.
A limiting factor of this study is that the HCP-–patient interactions are restricted to those recorded in the EPR system. There are two main areas of missing data one that can be more readily incorporated than the other. The first set of actions are the use of the EPR system when no data is initiated, for example, the reading of clinical notes, or just generally reviewing a patient’s notes without initiating a specific action. Access to the audit log of the EPR system may be able to address this area of missing data. The second area are interactions that do not involve the EPR system, for example, face-to-face conversations about a patient, multidisciplinary team meetings or visits to the patient’s bedside.
This study has focused on the visual analysis of HCP networks. The results of the study are likely to be of significant interest for multiple applications related to categorising the types of care given to an individual patient, using the variation in HCP network structure. Another area of interest could be to process the data for an individual admission as a single temporal network analysis. This approach is fundamentally different from standard database methods since it uses the relationship between the daily HCP networks, and further work will determine usefulness and applicability across a range of clinical scenarios.
[ad_2]
Source link