[ad_1]
Results
In total, we examined mortality patterns in 607 980 SoS patients across three Trusts. In Trust A, we included 156 387 patients who were admitted over 119 months, in Trust B 248 301 patients over 85 months, in Trust C 203 212 over 118 months and Trust D 110 110 over 46 months.
In all Trusts, the SoS cohort had more females than males, with a high proportion aged 65 and over, and the majority exhibiting at least one comorbidity. Admission rates were lowest between 20:00 and 07:00. The admission rate was similar in the winter and non-winter months. Approximately 40% of SoS patients at Trusts A, C and D are coded as white British and Irish, compared with nearly 80% in Trust B. We included all patients, even those with missing ethnicity; ethnicity was not known (either not stated or missing) for approximately one-sixth of patients (see table 2 for more details).
Summary of patients admitted with the SoS before and after the introduction of a sepsis screening tool
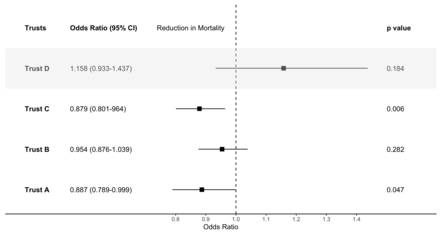
Trusts A, B and C had significantly lower mortality after the introduction of the sepsis screening tool before adjustment for pre-existing trends or patient casemix. After adjusting for pre-existing trends, there was a significant reduction in mortality in Trusts A and C, as shown in figures 1 and 2.
ORs for the impact of the introduction of a sepsis screening tool, adjusted for pre-existing trends, but not for casemix.
30-day mortality trend in the SoS cohort. Dots represent the actual mortality, the dashed line represents the counterfactual if there was no intervention and the solid line represents the modelled mortality pre the intervention, and post as if there was no intervention. SoS, suspicion of sepsis.
In Trust A, crude analysis indicated that there was a reduction in the mortality rate following the introduction of the screening tool (see figure 1). After adjusting for time and season of admission and patient casemix, the screening tool showed no impact on mortality (see table 3 for more details). We investigated whether the alert had differential impacts on specific patient groups by fitting interaction terms. This suggested that the introduction of the screening tool was significantly associated with a reduction in mortality in older patients, but not younger patients (see online supplemental table 2 for details). There was no evidence of a different impact on patients with more comorbidities.
Interrupted time-series analysis of the impact of sepsis screening tools on mortality outcomes for SoS patients in three NHS Trusts in England
In Trust B, prior to the introduction of a DSA there was a decreasing trend in mortality in patients in the SoS cohort, and the association of the introduction of the alert with mortality is not significant in both crude and adjusted analyses. However, the interaction between age and the introduction of the alert is significant, suggesting that the alert had a significant impact on reducing mortality in older patients, but not in younger patients.
In Trust C, there was an increasing trend in mortality prior to the introduction of a DSA, and an increase in odds of mortality of 2.6% (95% CI 1.2% to 4.0%). The introduction of the alert is associated with a decrease in odds of mortality of 14% (95% CI 21% to 5%). In addition, after the introduction of the alert, the trend in mortality rate changes to a decreasing mortality rate. However, there was no significant interaction between the introduction of the alert and age, suggesting the alert does not have a differential impact in patients of different ages.
The introduction of the EPR in Trust D was apparently associated with increased odds of mortality of 27% (95% CI 0.6% to 60%). We propose that this is likely to be to do with coding and recording changes as a result of both the introduction of the EHR but also national sepsis coding guidelines in April 2017 and again April 2018, which have been shown to have centre-specific impacts on mortality.17
While the primary objective of the statistical models is to assess the impact of digital sepsis screening alerts following casemix adjustment, the significance of various casemix variables presents an intriguing and complex pattern. The risk of mortality rises with age over 18 and higher Elixhauser scores. Being female is associated with a decreased risk of death. Additionally, mortality risk increases when patients are admitted during winter and not in the morning. The influence and significance of ethnicity on the risk of mortality exhibit variations across trusts. For example, being Asian or Asian British was associated with 20% higher odds of death in Trust A (95% CI 10% to 32%), a 29% lower odds of death in Trust B (95% CI 13% to 42%) and no significant association with mortality in Trust C. In addition, night-time admissions had a higher risk of mortality, across all Trusts.
Control cohort
To determine if any change in mortality rate was specific to patients with an infection rather than patients who are acutely deteriorating, we modelled mortality in patients with a gastric bleed, who did not also have an SoS diagnosis. There was no statistical evidence (p>0.05) that the introduction of sepsis screening tools was associated with a decrease in mortality in this cohort. Both increasing age and Elixhauser score were significantly associated with increased risk of mortality (see online supplemental tables 3,4 for more details).
Sensitivity analyses
Sepsis incidence: We investigated whether our hypothesis that the introduction of DSAs and financial incentives associated with sepsis screening affected the number of people with a sepsis diagnosis, which would justify our approach of using patients with a diagnosis from the SoS code list, rather than patients with an ICD-10 code specifically for sepsis. We found that the incidence of sepsis increases when a sepsis screening tool is introduced, and again when the coding policy changed in England. Although the number of patients who died during these times also increases, the case fatality is less (see online supplemental figure 1).
Additional adjustment for deprivation
Only two trusts provided data on deprivation. Including this in the model had no effect on the overall model interpretation. Patients with no deprivation recorded had the highest odds of death. For patients with a score, there was no significant association with mortality.
[ad_2]
Source link